The skin of children is gentle and sensitive. They need special to remain safe. Still, many childhood diseases are caused by bacteria or viruses.
There are several skin rashes that can harm your children. So, it is a discreet decision to take a rash of any kind seriously and visit pediatricians as soon as possible. There are common childhood skin rashes including eczema, diaper rashes that can lead to itchy, irritated skin.
These rashes are mainly due to sunny weather, stuffy climate, and balmy weather. Continue reading the ensuing passage to know more about them.
The different skin rashes in children
Check out the following points to get acquainted with types of skin rashes in kids so that you can prevent, identify and soothe these childhood skin problems.
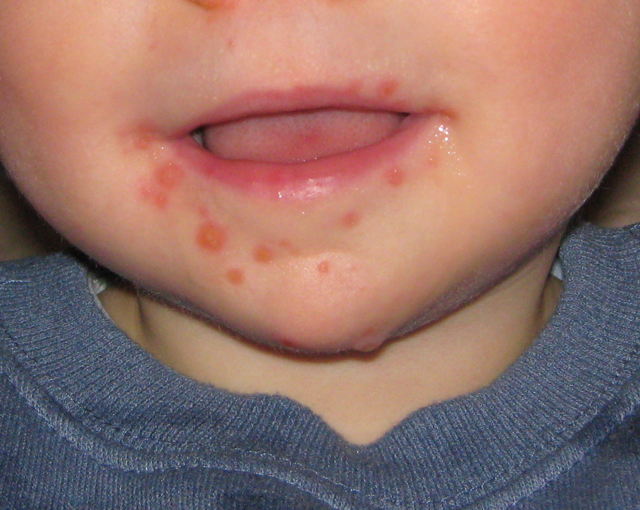
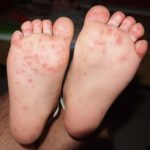
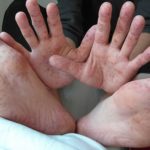
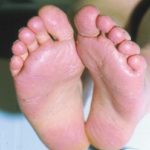
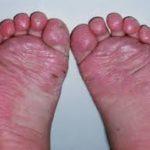
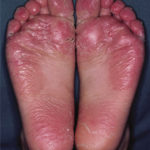
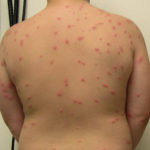
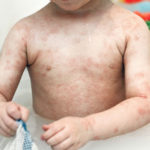
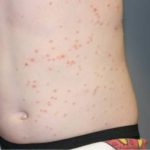
Hand, Foot and Mouth Disease (HFMD)
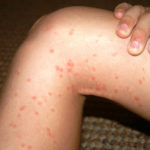
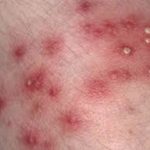
It is a common viral infection that is mostly found in children and kids. Painful and irritating red blisters appear in the mouth, throat and on the hands. HFMD is infectious and easily spread through the dirty hands, saliva (spit), feces (poop) or fluid from the blisters.
The kids under 5 years of age are at risk of suffering from HFMD. Blisters accompany with fever for a few days. The infected kids feel dehydrated as painful blisters hurt them to swallow liquids.
Symptoms include
- The soles of the palms of the hands have rashes that can appear like red spots or red blisters.
- Only want to have cold fluids
- Affected start drooling (for painful swallowing)
- Become irritable or sleep more than usual
- Decreased urine output
- Fever
- nausea
- vomiting
- feeling tired
- loss of appetite
- irritability
Prevention
Call your pediatrician if your children have a fever for more than 3 days or cannot take fluids. If the symptoms continue to be severe, the doctor will collect samples for lab testing.
Children suffering from hand, foot and mouth disease should drink plenty of fluids. Consult the doctor if your child is dehydrated.
The pediatrician may recommend acetaminophen or ibuprofen to relieve pain and fever. Liquid mouth-soothing alternatives are helpful to ease mouth ulcer pain.
Inform your child care providers and playmates’ guardians of the child to observe the symptoms of the ailment. The infected can spread this disease through the respiratory tract (lungs, mouth, and nose).
So, it is important to watch the people come in close contact with him or her. After the fever decreases, infected kids need not remain at home.
Juvenile Plantar Dermatosis (Sweaty Sock Syndrome)
Reddened, smooth rashes may appear on your child’s feet with cracking skin or scaly skin, peeling. These conditions are for Juvenile Plantar Dermatosis (Sweaty Sock Syndrome). These appear when the feet get wet and then dry quickly- mainly when one takes on and off the shoes during summer times.
Prevention
You can apply moisturizing ointment or over-the-counter steroid cream on the affected area of your child’s feet after taking off the shoes. If the conditions continue to be worse or you notice a sign of infection consult a pediatrician.
Select footwear made of the materials like cotton or mesh and more absorbent cocks. Also, be careful that your child’s feet are clean and remain dry.
Swimmer’s Itch
Also known as digger’s itch, this may occur after playing in lakes, ocean, and other water bodies. The rash is due to microscopic parasites in shallow, warm water bodies where children love to stay.
These parasites burrow into the skin, causing small reddish spots on the skin not covered by the swimsuit. Welts and blisters may also appear in the uncovered area such as hands, feet.
Prevention
Use home treatments such as cool compress on the affected area. Using Epsom salt or baking soda paste help to relieve the discomfort. If these treatments are not effective and symptoms continue to be severe, consult your pediatrician. He or She may suggest lotions or creams to reduce the symptoms.
Stay away from swimming or wading in marshy areas where snails are easily found. Do not attract birds by feeding where your kids are spending time. Birds eat snails and spread parasites in the water bodies.
Stop rubbing the towel on your child and keep the towel dry. The parasites burrow your child when you rub the towel on him or her. He or she can suffer from discomfort and rashes.
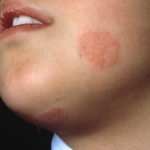
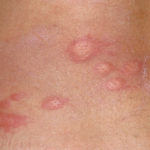
Tinea (Ringworm)
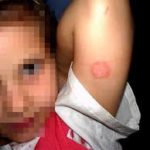
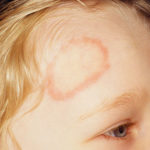
Tinea (ringworm) is an infection that is caused by a fungus that lives mostly in warm, damp conditions. This is similar to jock itch or athlete’s foot. It is termed as ringworm as the rash from the infection appears to be like round or oval shapes. The fungus can spread quickly among student-athletes, during the sweaty, summertime practices and games.
Prevention
Consult your pediatrician if you find a single ringworm patch on the skin of your child. He or she will prescribe stronger medicine if the rash is getting worse.
Check and treat the pets that can spread the fungus. Do not let your children share combs, brushes, hair clips, hats. Ensure the disinfection of the mats used in sports like wrestling, gymnastics.
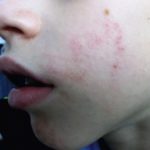
Poison ivy and other plant rashes
Many kids can develop burning, prickly rashes while they come in contact with plants such as poison ivy, sumac, poisonous oak as these plants contain a sticky oil called urushiol. Other plants like wild parsnip, giant hogweed containing phytophotodermatitis rash also cause skin rashes. The allergic skin reaction cause blisters, redness.
Prevention
Teach your children how these plants look and how to avoid them. Like, both poison oak and ivy have shiny leaves. If you have younger children, then ensure the park is free from skin rash-causing plants.
If the mild rash is found, then apply calamine lotion. Avoid ointments with antiseptic and antihistamines that are allergic to themselves. Visit the pediatrician if symptoms are severe.
Eczema
Eczema is a common in children that causes dry patches, scaly red skin. It tends to flare up during colder months. But dryness is due to air-conditioning. Travel during the summer times can cause such problems. Overheating, chlorine in swimming pools, sweating can trigger eczema.
Prevention
Choose clothing made of breathable, soft fabrics like cotton if possible. Wash clothes in a detergent free of irritants like dyes and perfumes.
Always keep your children’s fingernails short, and remind them not to scratch. Scratching can lead to infection and can make the rashes worse.
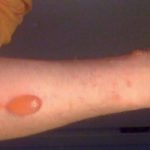
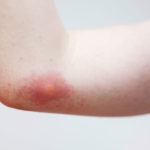
Insect stings and bites
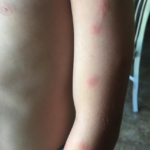
Irritating insects such as mosquitoes, ticks, fire ants cause minor uneasiness and itching among kids when they prick their skin. Sometimes, diseases like Lyme disease, Zika virus can be spread through these insects and cause rashes. For some children, insect bite and stings cause an allergic reaction called anaphylaxis that includes rashes and airway swelling.
Prevention
If spending time outdoors, avoid scented soaps and shampoos as they attract insects. If possible, avoid areas with insects’ nests and gather.
Wear light-colored garments to easily spot the ticks. After coming indoors, check your child’s skin to spot ticks as they often hide behind the ears or along the hairline.
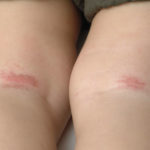
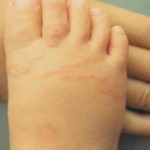
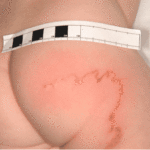
Cutaneous larva migrans (Sandworms)
Sandworms can appear in sand contaminated with fences from stray animals or pets. When a child comes to stand or sit in contaminated sand in a sandbox or on a beach, the worms may silently attack them. Lines of itchy, reddish rash known as creeping eruption appear. The condition is more common among the tropical and subtropical areas.
Prevention
If you are on an outing with to a pet-friendly beach, ensure that your child keeps shoes and do not sit in the sand without a towel or blanket.
Your pediatrician may suggest anti-parasitic medications such as albendazole or ivermectin for treating the rash.
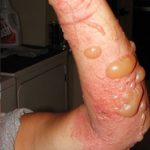
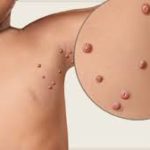
Molluscum Virus
It is a viral infection that can cause pearly bumps on the skin on your child’s back, chest, arms or legs. Also known as “water warts”, this bumps are common in humid, hot climates. This infection can spread in contaminated swimming pools.
Prevention
The child suffering from molluscum contagiosum should not share towels, clothing to avoid spreading.
Scratching the bumps can spread to another. So, avoid scratching them.
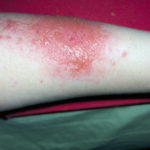
Folliculitis (Hot Tub Rash)
It is an itchy, pimply rash occurring when bacteria in dirty pool and hot tubs enter hair follicles on the skin. The hair-growing areas get affected and small, pus-filled blisters can appear. A similar rash can come out after wearing a damp swimsuit.
Prevention
The best thing is to steer clear of dirty pools. Don’t allow your child to enter such a pool.
Contact the pediatrician if the symptom worse.
Protecting your child’s skin throughout the year is important. Fortunately, some rashes clear up on their own. But it shows the signs of infection and shortness of breath, immediately consult a pediatrician.